Give us a call to discuss your problem or fill out the form below.
OR
Give us a call to discuss your problem or fill out the form below.
OR

Ankle arthritis is a medical problem that involves the interior surface of the ankle joint. This painful condition can be caused by normal aging or “wear and tear,” by an injury, or by inflammatory diseases.
The problem can involve the cartilage, the inner lining of the joint, as well as the bone foundation upon which the cartilage rests, ligaments that surround the joint, and the fluid within the joint.
Pain associated with ankle arthritis is often characterized as dull to sharp with the first few steps in the morning, and also in the evening after increased activities. Patients also report minor relief as it is “warmed up” during light walking and massage. Ankles that “give out” is also a common finding.

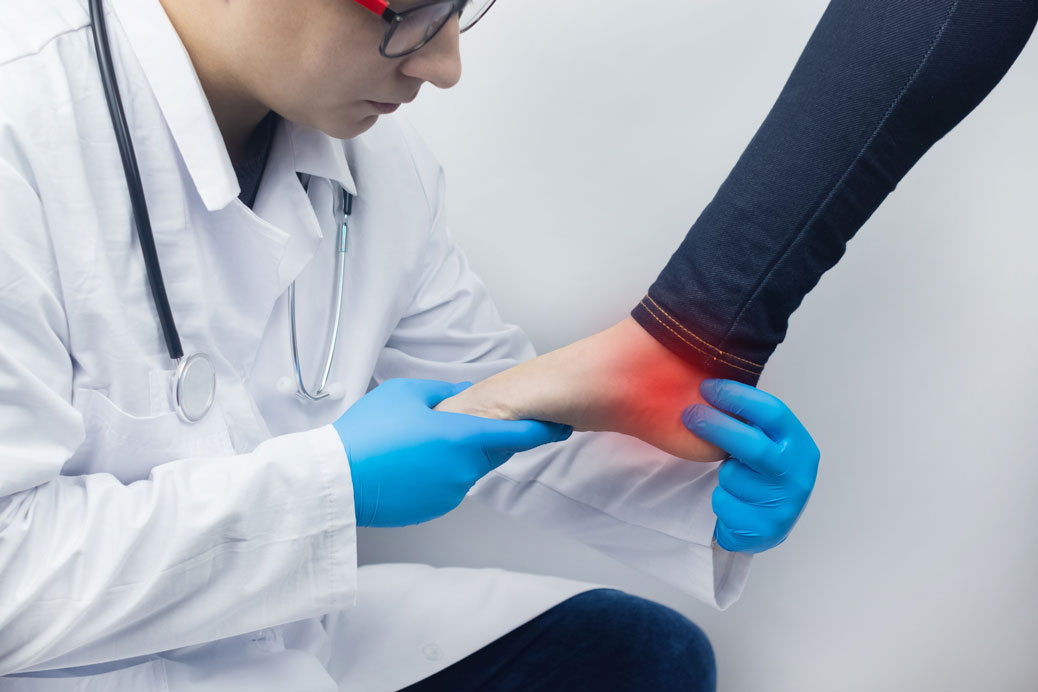
Each patient comes to us with different levels of pain, medical history, and lifestyle characteristics that can determine whether conservative treatment or surgical correction is right for them. If conservative treatment fails, the option to not have surgery is as important as the surgery recommended by your surgeon.
Oral anti-inflammatory medication can help with the chronic pain, but is not much help with the acute pain that comes with ankle arthritis.
Immobilization can vary from ankle bracing that allows some motion to complete immobilization with a walker boot. Temporary arch supports, supportive athletic shoes, and custom molded orthotics are a great way to reduce the amount of forces and excessive motion at the ankle joint and other supportive foot joints.
Cortisone can be directly injected into the joint where it can be most effective for relief. These injections can be administered with minimal discomfort.
Ankle arthroscopy is the gold standard for diagnosing problems within the ankle joint. It allows a small camera to go into the ankle through two small 1 cm incisions to the front of the ankle. Any damage to the ankle joint cartilage and inner joint wall lining is cleaned up and removed. Walking in a removable cast is allowed after 3 to 14 days.

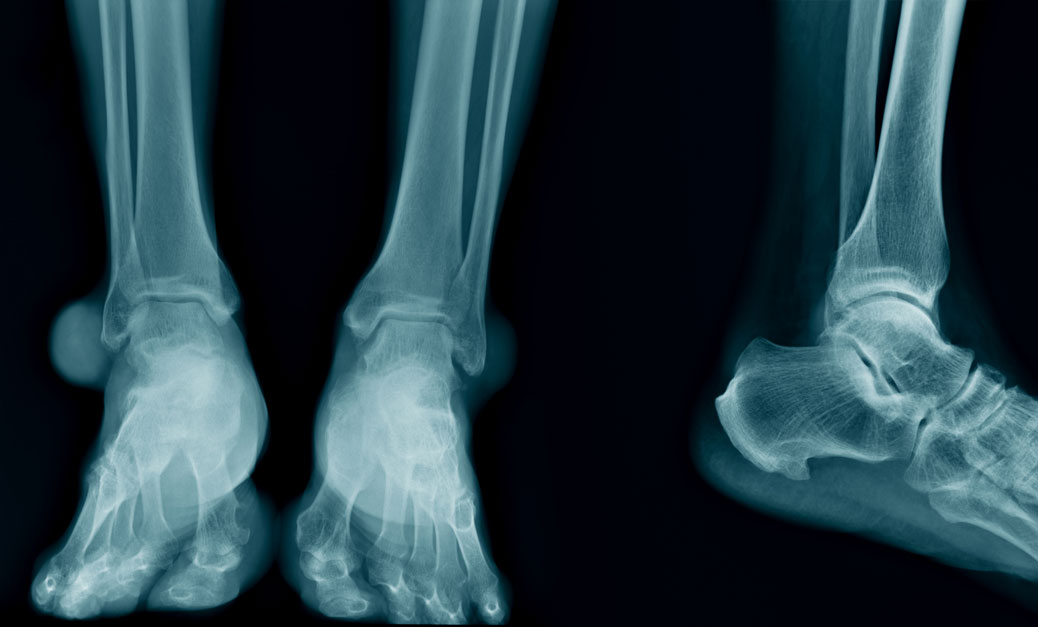
Ankle fusion is used to treat advanced arthritis and no relief of symptoms, restriction of joint motion, or severe joint pain. After removal of remaining cartilage from the joint surfaces, internal fixation fuses the joint slightly less than 90 degrees from the leg to allow the front of the foot to clear the ground when walking. Non weight-bearing in a cast is mandatory for 8 weeks and then full weight-bearing should be fine at 12 weeks if there are no complications.
Although many new ankle joint replacement devices are in production, the follow up studies and outcomes are not as successful as other joint replacement procedures like the knee and hip. Dr. Moore has opted to wait until better devices are on the market and does not perform this procedure at this time.
No, you wouldn’t consider ankle surgery a major surgery. Ankle surgery is performed in an out-patient setting, has minimal risk, and requires minimal post-operative care.
The incision care and keeping the ankle dry takes 2 weeks. Partial weight-bearing and light exercise on a stationary bike or swimming begins after 3 to 4 weeks. Full weight-bearing and exercise, such as walking or using the treadmill can be performed at 4 to 8 weeks.
No, ankle surgery should only cause minor discomfort. Postoperative ankle pain can be controlled with anti-inflammatories or narcotics like hydrocodone. A “popliteal block or catheter” is a pain-free postoperative option that you can utilize for the first few days after surgery.
Screws inserted during ankle surgery do not have to be removed. Healed bone is stronger than the equipment used to hold it together during surgery. If the screws become prominent or back out of the bone and become irritating or painful, then removal is warranted.
Patients can walk anywhere from 2 to 3 weeks after a standard Arthroscopic procedure. More extensive ankle surgeries can take up to 6 to 8 weeks before patients can walk.
Ankle surgery has minimal risks, but like all extremity surgeries, risks can include: infection, deep venous thrombosis, pulmonary embolism, joint instability, prolonged joint pain, lack of normal function, contracture of wounds, failure of bones and wounds to heal properly, painful scar tissue, and permanent swelling that does not respond to treatment.
“Amazing staff! So friendly and kind. I have had two successful foot surgeries with Dr. Moore. I wouldn’t trust anyone else. I now am pain free! I highly recommend Dr. Moore.”
-Amy
Our patient had a history of ankle sprains. An arthroscopic examination is common for this type of patient to repair internal cartilage damage. The cartilage damage (common with sprains) causes pain inside of the ankle with activity which then tells the body to shut down the leg muscles, thus the ankle “giving out” more frequently. With the addition of a torn ligament found on MRI, he had the choice to have it repaired at the same time as the arthroscopic examination or at a later time.
Avoid a life of discomfort and pain — contact us today to discuss possible routes of treatment for your arthritis condition.
Order by Phone
